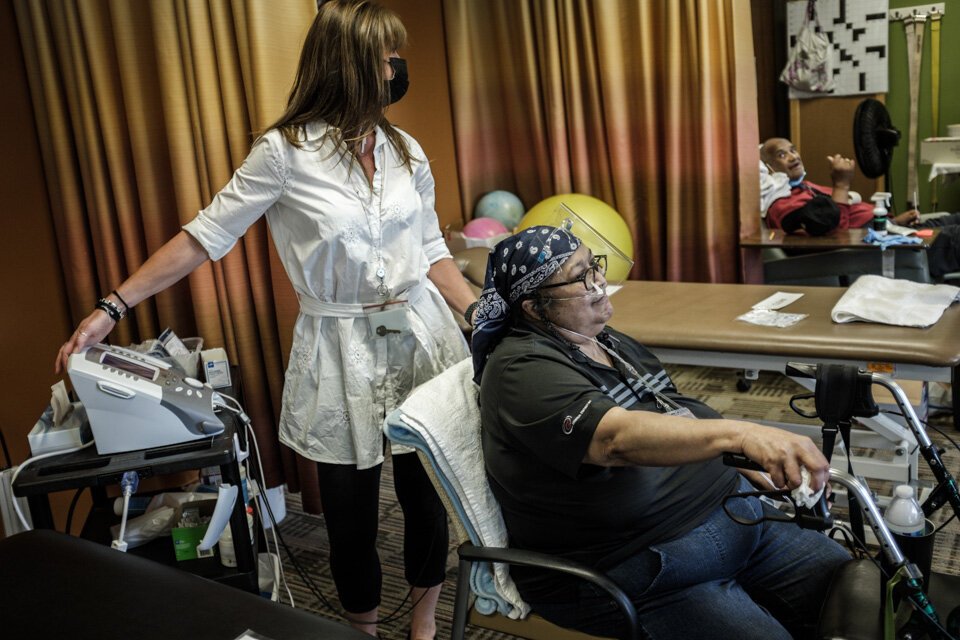
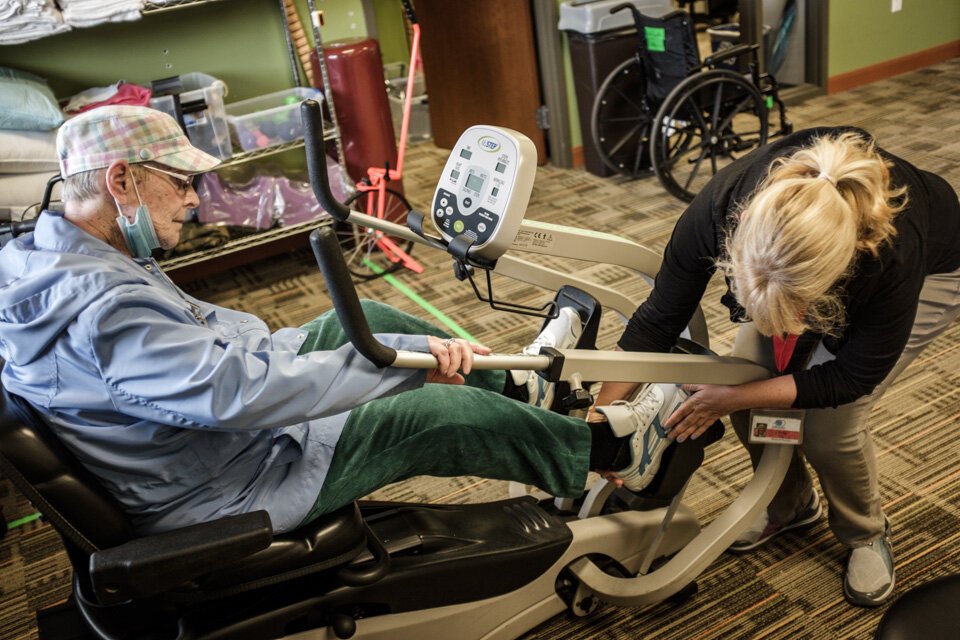
The COVID-19 pandemic has raised awareness about how Michigan communities can bridge gaps in care and improve quality of life for older residents.
This article is part of State of Health, a series about how Michigan communities are rising to address health challenges. It is made possible with funding from the Michigan Health Endowment Fund.
COVID-19 has taken a tremendous toll on Michigan’s older adults — not only because elders are more likely to die from the virus, but because social isolation, postponement of medical care, and reduced physical activity have diminished minds and bodies. On the bright side, the pandemic has raised awareness about how Michigan communities can bridge gaps in care and improve quality of life for older residents.
AARP Michigan, the PACE Association of Michigan, and local organizations like the Portage Health Foundation (PHF) are among those changemakers. A major focus for each of them is finding solutions that empower older adults to live longer in their own homes. AARP’s 2021 Home and Community Preferences Survey indicates that more than three-quarters of Americans age 50 and older want to stay in their current home.
“The risk of food insecurity and lack of healthy and nutritious food is one area [of need] that we’re seeing. Anecdotally, we’re seeing an increased demand for general health care, in particular end of life care, hospice care, and respite care,” says Kevin Store, executive director of PHF in Michigan’s Copper Country. “So many of our seniors have been locked down during the pandemic. There’s been a lot of chronic illness that has not been managed appropriately. Of particular concern for us is the decline in our elder mental health.”

To help address food insecurity, PHF took ownership of the region’s senior meals program. In addition to plans for expanding services to more older adults, the foundation hired a registered dietitian, a family medicine physician, and a functional medicine physician to the meals program staff.
“We want to assess the nutritional value as it relates to health and mental health issues that we know are prevalent,” Store says. “What foods can we incorporate that will help address mental illness or maybe Alzheimer’s?”
The program also leverages relationships with meal recipients to better identify other needs, for example, home repairs, housekeeping, or mental health issues.
“Our elder community accounts for about 12% to 13% of our overall population, but right now it’s accounting for about 18% to 20% of overall suicides. We’re seeing a 21% increase in suicides from 2019 to 2020,” Store says. “[Our older adults] are reporting a 20% increase in depression and anxiety and this is a population segment that historically doesn’t talk about those types of things.”
Helping Michigan catch up
According to Sarah Milanowski, enrollment manager for LifeCircles Program of All-Inclusive Care for the Elderly (PACE) in Holland and Muskegon, Michigan lags behind other states when it comes to supporting older adults who want to age in place. The PACE model provides comprehensive medical and social services at low or no cost to older adults who live at home. Fourteen independent PACE organizations serve 21 Michigan locations, covering more than 87% of the state. Even so, many older adults cannot find the supports needed to remain in their homes.
“We are lagging in [providing] home-based, long-term care for older adults compared to the rest of the nation,” Milanowski says. “I think it’s a lack of knowledge. We need to take a look at how the system is operating and be willing to make modifications.”

Milanowski relates the story of an older man who wanted to enroll in PACE so he could continue living at home. Because his Social Security and pension income exceeded Medicaid limits for home-based care by $300, he was forced to live in a nursing home, where Medicaid covered costs that his income could not. In addition, Michigan Medicaid timelines require older adults applying for PACE to wait until the first of the month after they are approved for services, leaving some who are in need of immediate home-based care waiting for up to eight weeks before help arrives.
“We also are trying to educate health care providers. Sometimes they are really nervous about sending someone home after a hospital visit,” Milanowski says. “The conversation could be a little more nuanced around Mom and Dad’s mental health, and the value of being in their own home versus going into a traditional facility.”
To make living at home a more viable option, Milanowski would like to see more resources devoted to making older adults’ homes more livable and preventive home maintenance services that keep the home safe for healthy occupation. She says investing in keeping older adults in their own homes would decrease their costs and the state’s costs for housing older adults in long-term care facilities.
On Dec. 1, 2021, AARP Michigan staff testified before the Michigan House Appropriations Committee about the need for more in-home care for older adults. They shared findings from an EPIC-MRA survey that found 89% of Michigan voters want to avoid ever living in a nursing home. And they noted that Medicaid dollars could support nearly three older adults in home and community-based services for every one person in a nursing home.
“When we look at the taxpayer dollars that get spent on long-term care services, 68.5% of Michigan’s Medicaid spending for long-term services and supports goes to pay for care in nursing homes instead of in people’s homes, where they want to be,” says Lisa Dedden Cooper, manager of advocacy for AARP Michigan. “Basically, the Michigan long-term care system is locked in this broken cycle in which we continue to spend too much taxpayer money for care in the settings that are both more expensive than alternatives, and not what residents want for themselves and their families.”
Bias against home care at the root
Cooper faults an institutional bias in the system that presumes a nursing home is the normal place people go when they need help with self-care tasks as they age. This bias also influences older adults and their families, leading them to believe institutional care is the best or only option. Those who go against the grain by choosing to stay in their homes often face waiting lists, income and asset tests, limited insurance reimbursements, and push-back from well-meaning health care providers that makes their choice even more difficult.

“Part of it is that the funding for [in-home] programs is limited compared to demand,” Cooper says. “Some of it are these enrollment barriers, including caps, and some of it is a limited supply of care options and more desirable alternative residential settings. Another one of the issues is with direct care workforce shortages.”
Cooper applauds the Michigan Department of Health and Human Services for looking at ways to increase the number of direct care workers, including home health aides. These workers tend to work very hard for low wages and little respect while performing tough tasks like lifting patients, bathing them, and changing their diapers.
“There’s not any kind of career path and usually no benefits that these workers get,” Cooper says. “So part of the work is to look at what we can do to create a more sustainable direct care workforce moving forward. Higher wages are part of it, but also things like opportunities to provide benefits, career paths, training, and credentials.”
The state of Michigan is also looking to make positive changes for older adults via its Health and Aging Services Administration (HASA). Established in October 2021, HASA will provide more coordinated services to Michigan’s growing aging population. Nearly 25% of the state’s population is over age 60, with those age 85 and older being the fastest-growing age group.
“I think the state is keyed into the deficiencies in the current system. And at the same time, there is this new funding that’s available from the federal government to try to put in place some changes, systemic changes,” Cooper says. “I’m hoping that there is going to continue to be momentum with policymakers.”
A freelance writer and editor, Estelle Slootmaker is happiest writing about social justice, wellness, and the arts. She is development news editor for Rapid Growth Media and chairs The Tree Amigos, City of Wyoming Tree Commission. Her finest accomplishment is her five amazing adult children. You can contact Estelle at Estelle.Slootmaker@gmail.com or www.constellations.biz.
LifeCircles photos by Pat ApPaul. Kevin Store and Lisa Dedden Cooper photos courtesy of the subjects.